Staff burning out? Who is Responsible?
Overwork and fatigue are increasingly prevalent issues in healthcare.
While it’s easy to tell people to take a break, you might be treating the symptom not the overall problem - workload management and work design.
Burnout rarely occurs from a single, stressful day, instead developing when work design consistently requires staff to operate beyond sustainable limits.
Kendall Schutz, Founding Director of Nexus Co Solutions, explains:
“Having a psychological safety policy in place, which commits to monitoring and controlling workloads, so employees are not pushed beyond safe limits, is key.”
“This could include strategies like adhering to safe hour guidelines, ensuring adequate staff coverage so individual scan take their entitled breaks, and using rostering practices that allow for recovery time between intensive periods.”
“Staff should be actively encouraged to use their annual leave and providing backfill to do so is another important practice for healthcare providers.”
Burnout isn’t an individual responsibility
A Mental Health Australia survey of healthcare workers in 2022 found 84 per cent were experiencing burnout.
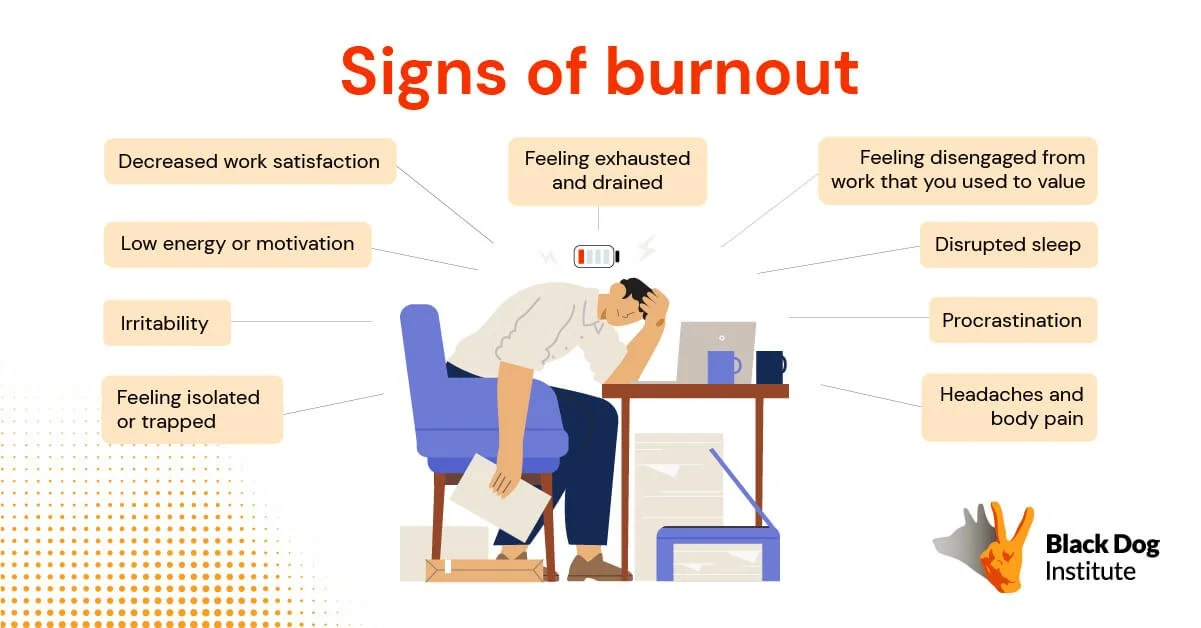
Burnout is a psychosocial hazard, something that could harm someone’s mental health, cause stress or physical harm. The Black Dog Institute highlights the below as signs of burnout.
Feeling drained
Feeling fatigues by work
Disengagement from work
Reduced sense of accomplishment
Feeling ineffective
Irritability
Headaches and body pain
Disrupted sleep
The impact of work design
Stress is a part of life, and in a high pressure environment like healthcare, the need to have a well structured work design can reduce the potential for burnout to develop.
Schutz says providers should take a close look at how the systems within their organisation operate.
“It could be as easy as creating a policy to rotate assignments so the burden for high-stress jobs doesn’t solely rest with one person or even ensuring you’ve got cover for peak stress periods, like the flu season, so staff feel they can take the time they need to look after themselves.”
“Making these systemic changes can be hard, but prioritising the wellbeing of your staff is important for them as individuals, your workplace culture, and importantly, the quality of care you provide to others.”
Recently, a nurse in New South Wales was awarded more than $1.2 million in damages after the District Court found her employer breached its duty of care.
The nurse sustained a serious injury while assisting with patient handling at the end of the shift.
The findings were not about individual error or competence. rather about how staffing levels, workload expectations and fatigue made safe work realistically achievable within the hospital.
“This reinforces what we know now - harm happens when the system of work makes risk foreseeable.”
Giving staff the power
Schutz says creating a safe workplace links in with creating a strong climate where employees feel empowered to speak up.
“Ensuring your staff know they can talk if the workload is unmanageable or they’re feeling fatigued without feeling like they’ll be disadvantaged is pivotal to the culture of your workplace.
You value your staff as people, and their safety - as well as that of their patients - must come first and the system should support them.
Ultimately, by committing to manage workloads and design work thoughtfully, the organisation is addressing of the most critical psychosocial hazards in healthcare at its root.”